Randomized Trial of Bilateral versus Single Internal- Thoracic-Artery Grafts

BACKGROUND
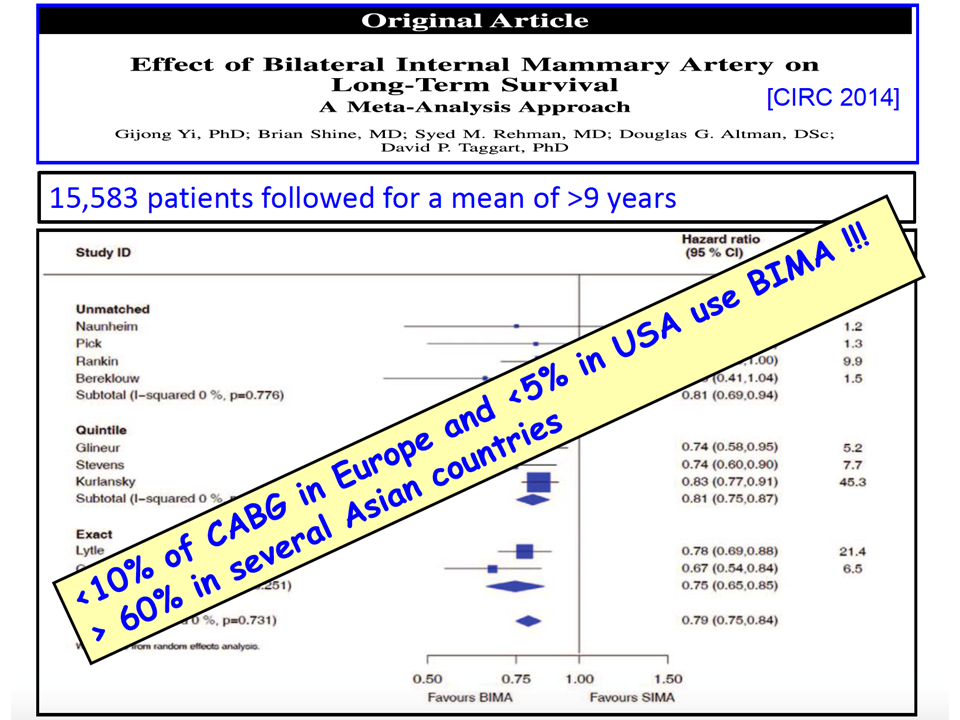
The use of bilateral internal thoracic (mammary) arteries for coronary-artery bypass grafting (CABG) may improve long-term outcomes as compared with the use of a single internal-thoracic-artery plus vein grafts.
RESULTS
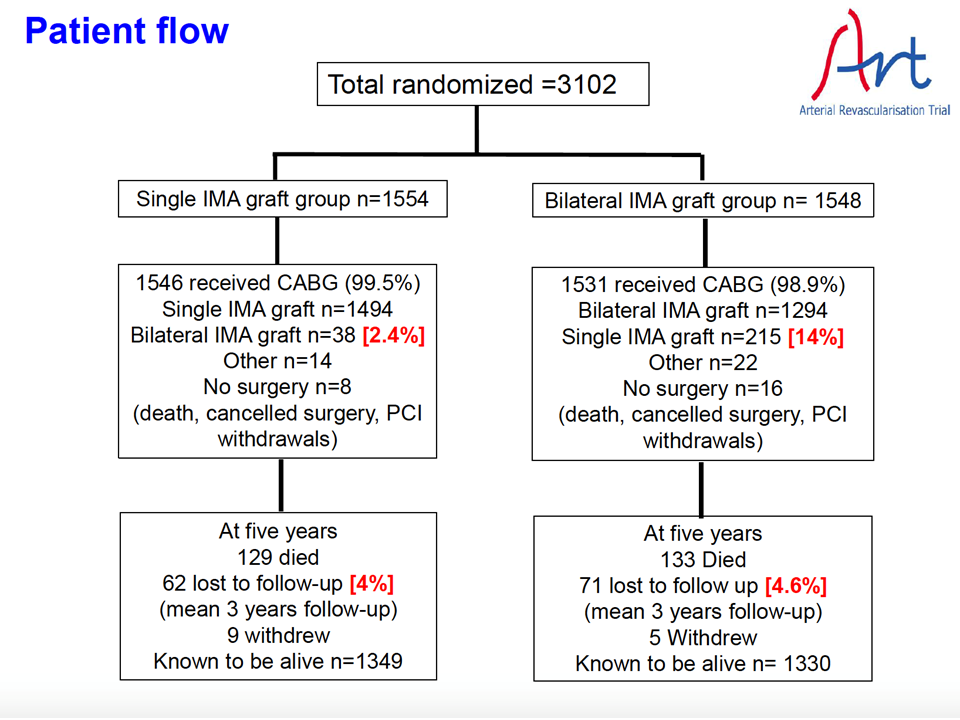
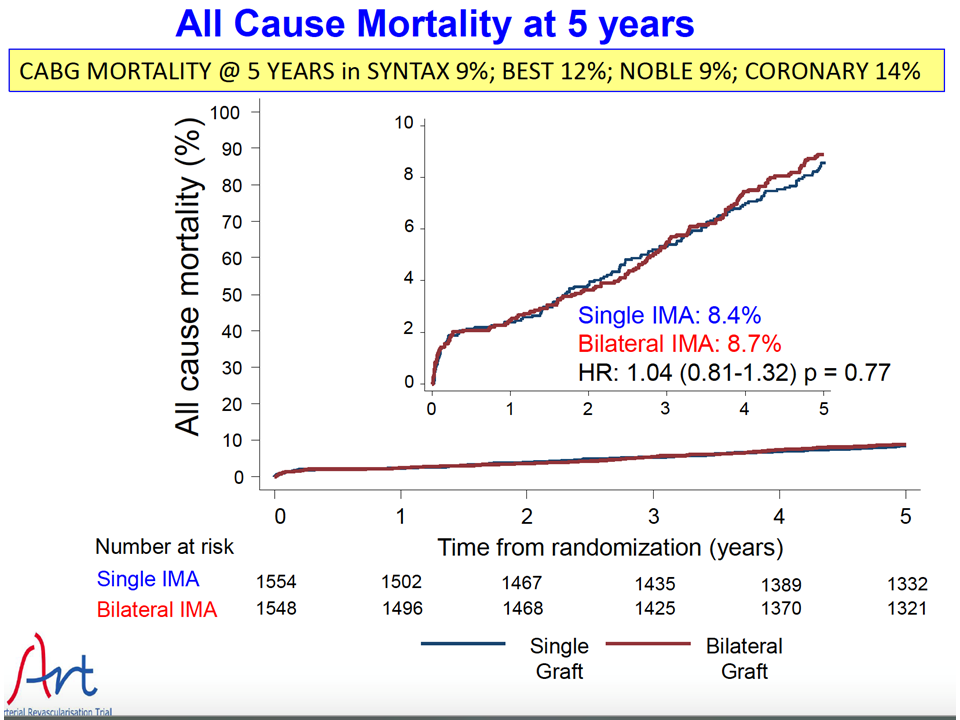
A total of 3102 patients were enrolled; 1554 were randomly assigned to undergo single internal-thoracic-artery grafting (the single-graft group) and 1548 to undergo bilateral internal-thoracic-artery grafting (the bilateral-graft group). At 5 years of follow-up, the rate of death was 8.7% in the bilateral-graft group and 8.4% in the single-graft group (hazard ratio, 1.04; 95% confidence interval [CI], 0.81 to 1.32; P = 0.77), and the rate of the composite of death from any cause, myocardial infarction, or stroke was 12.2% and 12.7%, respectively (hazard ratio, 0.96; 95% CI, 0.79 to 1.17;
P = 0.69). The rate of sternal wound complication was 3.5% in the bilateral graft group versus 1.9% in the single-graft group (P = 0.005), and the rate of sternal reconstruction was 1.9% versus 0.6% (P = 0.002).
CONCLUSIONS
Among patients undergoing CABG, there was no significant difference between those receiving single internal-thoracic-artery grafts and those receiving bilateral internal-thoracic-artery grafts with regard to mortality or the rates of cardiovascular events at 5 years of follow-up.
There were more sternal wound complications with bilateral internal-thoracic-artery grafting than with single internal-thoracicartery grafting.
Ten-year follow-up is ongoing.